Life in long-term hospital “unbearable”: Montreal man with ALS
Published in Montreal Gazette July 15, 2020, written by Charlie Fidelman
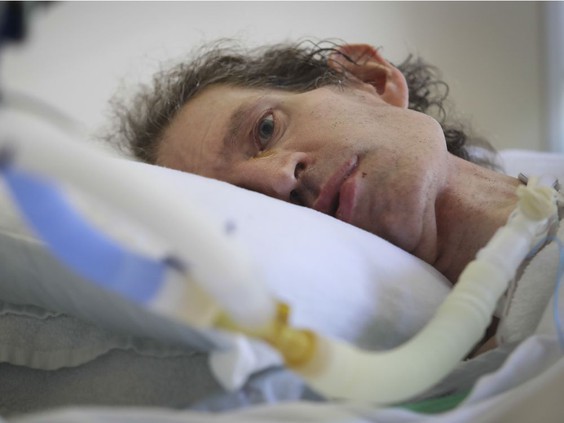
Archie Rolland in the Pavillon Camille-Lefebvre: Under Canadian and Quebec end-of-life guidelines, he qualifies for physician-assisted help in dying. His family supports his decision to end his life. PHOTO BY JOHN KENNEY /Montreal Gazette
A year after 18 patients with severe degenerative conditions were transferred to Lachine Hospital, some families say their care has degenerated.
Former Montreal landscape architect Archie Rolland says he would rather end his life than live in pain at a long-term care facility in Lachine that he says is treating him inhumanely.
“I am suffering too much to live,” Rolland, 52, who has ALS, or Lou Gehrig’s disease, told the Montreal Gazette last week.
Rolland plans to move out of the Lachine Hospital’s Camille-Lefebvre wing next week in a private ambulance taxi — along with a ventilator, an extra battery, suctioning kits, feeding formula and medications — and go to the family cottage in the Lower St. Lawrence region.
He’s considering taking his last breath there, within days. Under Canadian and Quebec end-of-life guidelines, he qualifies for physician-assisted help in dying. His family supports his decision to end his life.
In his hospital room last week — toileted and fed and turned on his right side to relieve pressure wounds on his back — Rolland’s face contorted with tears when asked if there’s anything that would change his mind. The air in the room filled with the hissing of his ventilator.
Once a hockey player, sailor and equestrian, Rolland was in full stride when he got ALS in his mid-30s, a debilitating neurodegenerative disease that attacks the nerve cells. Most ALS patients die from respiratory failure, usually within three to five years, with few surviving for 10 or more years. Not Rolland. Although the disease paralyzed his limbs, speech, swallowing and breathing, family and friends say he has clung to life passionately since he was given the diagnosis 15 years ago.
It’s not the illness that’s killing him, Rolland said in a series of emails with the Montreal Gazette. He’s tired of fighting for compassionate care.
“The people here don’t understand ALS and can’t look after me. It is unbearable.”
Rolland is one of 18 patients with severe degenerative conditions and respiratory ailments who were transferred to the second floor of the Lachine Hospital’s Camille-Lefebvre wing when the downtown Montreal Chest Hospital of the McGill University Health Centre closed in January 2015 as part of the move to the Glen site.
It was not a happy move for all involved. Many of the families objected repeatedly to the transfer, calling it a forced relocation.
Patients’ families feared the move would destabilize patients, of whom 14 are on ventilators. Totally disabled and dependent on the institution for care, they moved from a specialized medical hospital to a long-term care ward with 22 aging residents.
In interviews with the Montreal Gazette last week, five families who show up daily to provide services to make up for staffing shortages say gaps in care are getting worse.
Staff is on a monthly rotation, call bells are ignored, and when agitated family members advocate for better care, they say they are threatened with eviction from the hospital. On Mother’s Day in May, Rolland’s mother challenged the feeding schedule in Archie’s care plan, and the hospital called security and barred her from the hospital. She hired a lawyer to reinstate her visiting privileges.
The hospital has zero tolerance for violent or threatening behaviour, Lachine interim associate director of nursing, Chantale Bourdeau explained. “She was yelling at the staff. I had to intervene,” she said.
Bourdeau dismissed charges that call bells are not answered in a timely manner. “This is not possible,” she said, adding that someone on the team “responds right away, within two minutes.”
Her staff is dedicated to the patients from the Chest, Bourdeau said, and is doing everything to provide them with the best care possible.
However, a trail of emails from Archie Rolland to the head nurse, the ombudsman, the head of human resources in geriatrics, a patient’s committee representative and other hospital officials document a litany of complaints concerning his care. In one incident, an assistant nurse failed to properly suction a thick mucous plug from his wind pipe and then ignored his ringing ventilator alarm until Rolland’s mother ran for help before his lungs collapsed and he went into respiratory failure.
“If my mother wasn’t there I might have died,” Rolland wrote in October, with additional comments from Rolland’s sitter, who confirmed witnessing similar delays in responding to alarm bells on at least two other occasions.
Rolland’s massage therapist said her client demanded water to moisten his lips but was left without for nearly three hours — because it wasn’t in the schedule.
Families say the next step is to lobby the provincial health department. They want staff dedicated to patients with critical, long-term health needs. The Lachine pavilion is better geared to aging residents with dementia, not sick, middle-aged medical patients — who are completely lucid but are hooked to life-saving devices. Also, scheduled care plans and rotating staff assure efficiency but lack flexibility to respond to patients’ needs or requests.
“It’s a unique facility. We have residents and patients. My children are patients,” said Carol Silver, whose daughter, 45, and son, 52, have myotonic dystrophy, a genetic disorder characterized by progressive muscle wasting and weakness. Families need to fight, but some are very demanding and will never be satisfied, Silver said, adding the facility is doing a good job “90 per cent of the time.”
Before the move, MUHC hospital officials told families not to worry because the same nurses and orderlies familiar with their needs were also transferring from the Chest. But hospital officials confirmed last week that only 70 per cent of the nursing staff made the transfer, and fewer than half the hospital attendants or orderlies, known as PABs.
To harmonize care, the hospital is rotating staff through various wards every month; families were not consulted on this.
Bourdeau explained that new staff is trained on patient-care plans – plans that are created by multidisciplinary teams with the families. Patients aren’t handed off to untrained staff, she said. PABs work in pairs and one on the care team is always familiar with a patient’s routine, Bourdeau added: “They are never alone in a room, taking care of a patient that they’ve never cared for before.”
But families disagree. They say patients face a revolving door of orderlies.
“We were hoping things would improve with time, but it’s gotten worse,” said Luciana D’Amore, whose husband, Gian Libero Casale, 58, has locked-in syndrome and communicates by blinking his eyes. “There’s a constant change of people, and that creates a whole set of problems. Like guinea pigs in a bed – and us, the family are hostage, we can’t leave their bedside, because they won’t get the proper care.”
“Every day we have to adjust to new people who don’t have the training. When it goes bad for one of our patients, you have to turn around right away. Even when they are stable they are fragile. Not (just) anyone can look after them.”
Rolland touches his head to a bell placed by his forehead. Once someone comes to his bedside, he uses the eye-tracking mouse in his eyeglasses to type his request on hiscomputer. The disease destroyed his muscles and he is often in pain. Comfort lies in small details, from placing his head so it doesn’t flop to one side, near the call bell and in line with the computer, to the angle of the soft gel pillows under his ankles.
For six years, Rolland had a constant PAB at the Chest. After the move, he was re-assigned, despite Rolland’s pleas for continuity of care.
“It was unbelievably awful last night,” Rolland wrote in an email to his mother on June 6 about two PABs on his rotation.
“One left saying I wanted stupid things. She was leaning against the rail so that the bell jammed against my head and I couldn’t move or write. The one that stayed didn’t know anything and left me in a mess as her time (with me) was up and she did not return despite my ringing the bell. No one came for an hour and a half” to adjust his feet, the blanket or turn off the light.
“One of the night PABs laughed at me in my distress …” Rolland continued. “I was terrified to ask them to move me because they would just make it worse. Took Ativan and Dilaudid at a.m. but was so badly set up that I didn’t sleep all night.”
Archie Rolland in the Métis Gardens in 2000: Rolland, 52, is a former landscape architect who is in the advanced stages of ALS (Lou Gehrig’s disease). PHOTO BY COURTESY OF ROLLAND FAMILY
Dissatisfied with Lachine Hospital, Archie Rolland transferred for one month to Mount Sinai Hospital Centre, a respiratory, long-term and palliative care hospital in Côte St. Luc, but returned to Lachine in the spring because the facility was not set up to meet his needs. He says it has been downhill ever since.
His mother hasn’t endeared herself to the staff. She calls Archie’s hospital ward Guantanamo Bay, after the notorious military prison.
But Alison Rolland said she is not being demanding, and that hospital officials are shooting the messenger.
“They can say I’m difficult, but I’m fighting for his life,” she said.
Ewa Sidorowicz, MUHC director of professional services, said the Lachine facility has gone out of its way to accommodate the Chest patients and their families. But some families are “challenging” to deal with, she said.
“These are patients with complex medical difficulties. Their families are very protective of them and we understand that,” Sidorowicz said. “But it creates complex dynamics — sometimes within the families themselves and with the care teams.”
However, staff has been extraordinary in handling increased duties, she said: “Lachine has stepped up to the plate 100 per cent and is doing an amazing job for these patients.”
Asked to respond to Rolland’s statement that inhumane care is driving his wish to die, Sidorowicz said she was devastated to hear that.
“We’re going to be there if he needs us, depending on his decision,” she said.
Camille-Lefebvre is like other public long-term institutions, or CHSLDs, which face increasing demands for services in an era of financial austerity, said lawyer and patients’ rights advocate Hélène Guay, who got Alison Rolland’s visiting rights reinstated in early June.
“The director of nursing is good-hearted and a clinical nurse,” Guay said, but there is a lack of staff and resources across the board in such institutions. Patients like Rolland are seen as claiming more care than they are entitled to, she added.
Long-term institutions have made headlines recently because of residents’ demands for the right to have more than one bath a week.
The Quebec Ombudsman released a report in 2014 saying that more than 13 per cent of complaints about health and social services involved CHSLDs. It concluded that 51 per cent of complaints it received about CHSLDs were valid, compared to just 43 per cent of complaints for the health and social services sector as a whole. Over five years, the ombudsman intervened in 128 nursing homes – representing 63 per cent of all CHSLDs in Quebec.
Thirty-six per cent of the complaints judged to be valid concerned the quality of care and services, 23 per cent concerned the physical environment and the living environment and 16 per cent concerned non-respect of rights.
“The more care is required, the more the family is insistent,” Guay said. “But if he’s not comfortable, that’s the only thing that is important to him.”
Join our fight to #EndALS!
Sign up as to receive periodic email updates and join our circle of supporters!
